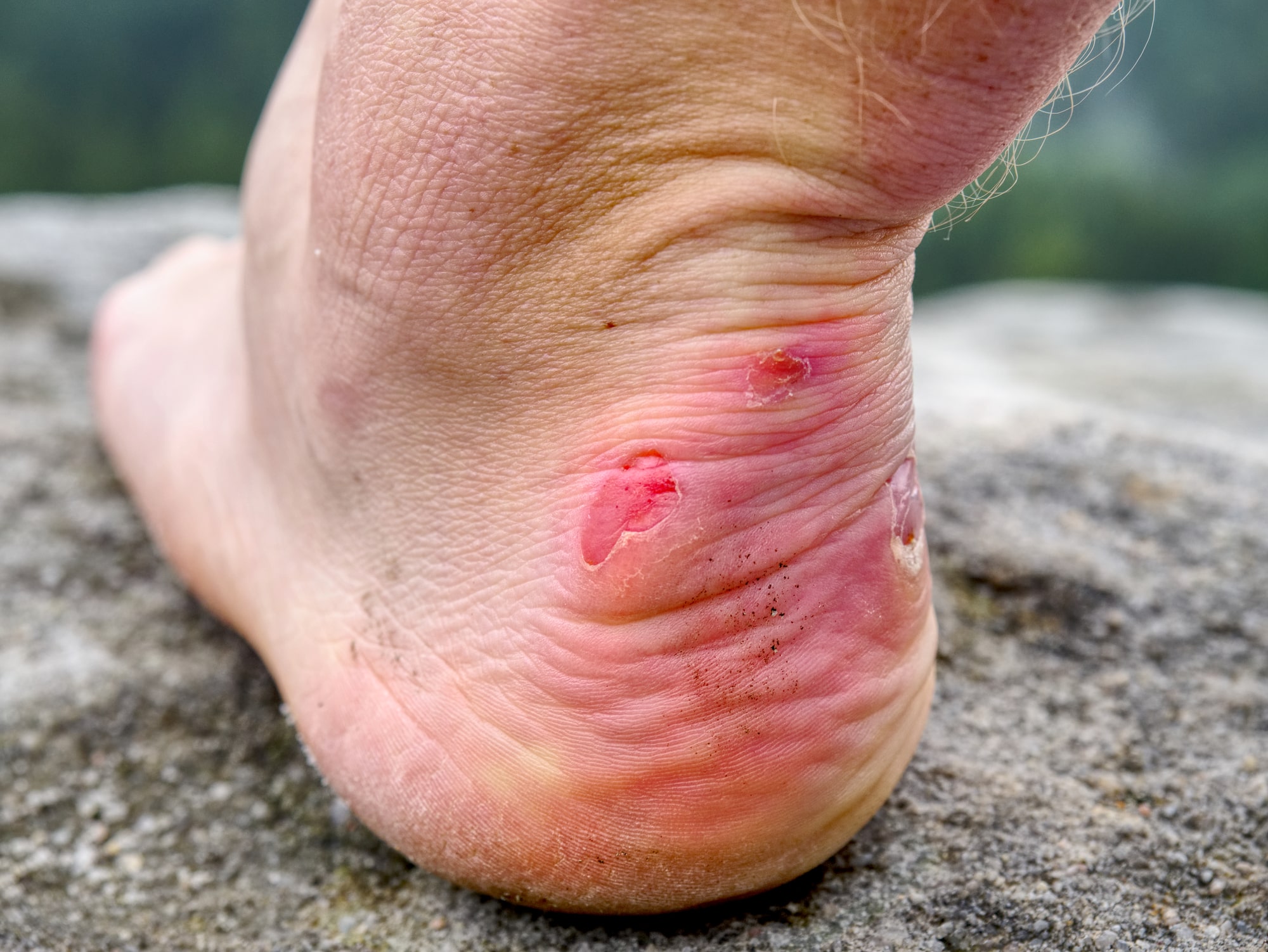
Several skin conditions are associated with diabetes, one of which is diabetic blisters. Diabetic blisters most often appear on the legs, feet, and toes. Though most cases clear up without complication, it is important to know the signs and symptoms of diabetic blisters so that they can be dealt with safely and appropriately. The biggest risk with diabetic blisters comes from a secondary infection, so preventative care and expert wound care play important parts in mitigating more dire risks.
Diabetic blisters, also known as bullosis diabeticorum or diabetic bullae, are twice as likely to be found in men as they are in women. They can be as large as 6 inches, though they’re normally smaller. The blisters look similar to those that occur on the skin after a bad burn. Although the blisters may be alarming when you first spot them, they’re painless and often heal on their own. However, due to the risk of infection and ulceration, people with diabetes who experience diabetic blisters should seek a consultation with a professional.
The good news is, in addition to usually being painless, the fluid in the blister is sterile. Diabetic blisters usually heal in two to five weeks without intervention. However, the following symptoms are a sign that you should visit your podiatrist immediately: redness around the blister, swelling, warmth radiating from the lesion, pain, and/or fever that accompanies the above symptoms.
To prevent infection, do not puncture diabetic blisters. Your podiatrist at Corona Foot and Ankle may recommend treatment with antibiotic cream or ointment and bandage to protect your diabetic blisters from further injury. Your podiatrist may want to drain larger lesions. It’s always especially important for diabetics to wear comfortable, well-fitted shoes as a preventative measure against the formation of diabetic blisters. The fungal infection Candida albicans is another common cause of blisters in people who have diabetes, so meticulous hygiene is critical. Having completed a thorough exam, your podiatrist may recommend a variety of treatments to speed up healing and relieve discomfort. For example, a saline compress can help relieve itching and irritation. A bandage, for example, may protect the blister and surrounding skin from bursting as a pre-mature puncture would increase the likelihood of infection. In more extreme cases, a podiatrist may recommend antibiotics or steroids topically.
Diabetic blisters may be a sign of a more serious skin situation. A good podiatrist would conduct a more thorough exam and even a biopsy to ensure the root cause of the issue is dealt with appropriately and expeditiously. One tip: It’s important to discuss all foot issues with your podiatrist. A reoccurring or nonhealing ulcer that causes severe damage to tissues and bone may require surgical removal, amputation, of a toe, foot, or part of a leg. Some people living with diabetes have a higher risk of serious side effects.
At Corona Foot and Ankle, our doctors are experts when it comes to diabetic foot care. We understand the intricacies of the healing process and how to promote wound healing and prevent reoccurrences. Our comprehensive exams are designed to address the true cause of your diabetic blisters, rather than simply masking symptoms, in order to promote long-term health. Unfortunately, people living with diabetes have an increased risk of lower limb amputation. As diabetic foot care experts, our doctors can diagnose and treat any issues early on so as to exponentially reduce the need for such extreme measures. If you suspect you may have a diabetic blister, or if you are living with diabetes and looking for expert foot care and preventative tools, contact us at Corona Foot and Ankle here as soon as possible.
Have any questions about treatment? Feel free to make an appointment, Our team will reach you soon!
Contact Us