
Approximately 1.5 million Americans are diagnosed with diabetes every year.[1] Unfortunately, diabetes is not yet a curable disease. Diabetes-related deaths were the 7th leading cause of death in the United States in 2015.[2] However, it is a very manageable disease and, treated properly, people with diabetes can live long, healthy, and happy lives.[3] Podiatrists play a key role in the early identification and treatment of foot problems in people with diabetes. In 2015, 30.3 million Americans, or 9.4% of the population, had diabetes.[4]
Type 1 and type 2 diabetes have different causes, yet both are influenced by genetics and the environment. You inherit a predisposition to the disease then something in your environment triggers it. Accurate and early diagnosis, as well as a balanced diet, exercise, and sometimes medicine, can help prevent or delay complications.
Often, regular care with a primary care physician should be supplemented with visits to specialists, like a podiatrist. One reason to consult regularly with a podiatrist is to minimize the risk of developing diabetes-related complications, which often present initially in the foot.[5]
A podiatrist would complete a comprehensive foot examination for abnormalities, including evaluation of pulses, sensation, biomechanics, and nails, as well as a footwear assessment. These evaluations help determine a patient’s category of risk for developing foot complications. People with diabetes have an increased risk of developing gangrene.
Gangrene refers to the death of body tissue due to either a lack of blood flow or a serious bacterial infection.[6] The most common form of gangrene develops in the feet of people with diabetes who also have associated loss of circulation in the feet and toes.
Those with diabetes have an increased risk of developing gangrene. High blood sugar levels can damage nerves, which may cause a loss of sensation in the affected area making it easier for an injury to go undetected. Typically, a sudden onset of pain in the feet or legs associated with a decrease in skin temperature, and color changes to the skin of the feet is a strong indication that there has been a sudden blockage of blood flow to the legs. However, people with diabetes may not experience the pain associated with such a sudden blockage due to a condition called diabetic neuropathy.
Diabetic neuropathy affects the nerves in the feet and legs causing a diminished ability to perceive pain, excessive heat, cold, vibration, or excessive pressure. This condition places people who have diabetes at greater risk of injury without their being aware of it.[7]
High blood sugar can also affect your blood vessels and limit the blood flow to your feet. As a result, fewer infection-fighting cells can make it to wounds that may develop on your feet resulting in a higher risk of infection.[8]
If the person with diabetes also has poor circulation, the infection can lead to gangrene of the toe. This situation can ultimately lead to the amputation of the toe, foot, or leg, depending upon how bad the circulation is in the leg.
I know of a recent case that began rather innocuously and ended disastrously due to a lack of proper monitoring a podiatrist can provide. In this case, an elderly patient with diabetes developed very dry skin on her feet that eventually cracked. This patient’s primary care physician did not address the issue immediately, nor did the patient visit a podiatrist. From the crack developed an infection, which due to diabetic neuropathy, the patient was unable to feel getting worse. It developed into gangrene and her status deteriorated rapidly, necessitating surgery. On the day of the surgery, her hemoglobin levels dropped, requiring a blood transfusion. The day after the surgery was performed, the patient applied pressure to the wound and her stitches opened up. Thankfully, she is finally recovering. However, these drastic measures and trauma could have been avoided had she been properly monitored and received preventative care from a podiatrist.
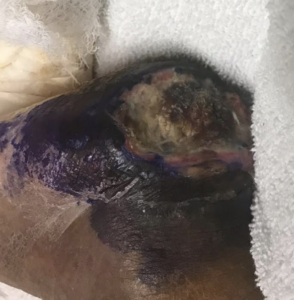
Treatments for gangrene include surgery to remove dead tissue, antibiotics, and hyperbaric oxygen therapy. The prognosis for recovery is better if gangrene is identified early and treated quickly. I focus on getting to the root problem and preventing recurrence; prevention and education are crucial. Podiatrists are important in the collaborative inter-professional team care approach for diabetes management.[9] I am a board-certified podiatrist serving the Inland Empire, and surrounding cities and the nearby county’s like Orange County, Los Angeles County, and San Diego County. I work with patients of all ages to provide the unique monitoring, prevention, and care that diabetics require.
[1] http://www.diabetes.org/diabetes-basics/statistics/?loc=db-slabnav
[2] http://www.diabetes.org/diabetes-basics/statistics/?loc=db-slabnav
[3] http://www.diabetes.org/diabetes-basics/?loc=db-slabnav
[4] http://www.diabetes.org/diabetes-basics/statistics/
[5] https://www.cdc.gov/diabetes/ndep/pdfs/ppod-guide-podiatrists.pdf
[6] https://www.mayoclinic.org/diseases-conditions/gangrene/symptoms-causes/syc-20352567
[7] http://www.podiatrynetwork.com/common-disorders/14-foot-disorders/63-gangrene
[8] https://www.healthline.com/health/gangrene-diabetes#diabetes
[9] https://www.cdc.gov/diabetes/ndep/pdfs/ppod-guide-podiatrists.pdf
Have any questions about treatment? Feel free to make an appointment, Our team will reach you soon!
Contact Us